I am not a doctor or anatomy expert. The following information is presented more or less in layman's terms because that is the terminology I understand. Any misinformation or exaggeration is because I don't know everything about everything yet. But hey, you are here and this is my blog. Jeremy Run's This. Feel free to comment and correct anything I screw up but as far as I understand and am willing to understand currently the following is true. I provide it partially for my own record but also so that those who care will have one (hopefully) consistent account of my vein journey.
Anatomy Lesson #1
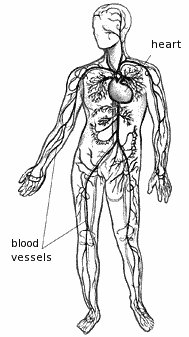
 The human body has miles and miles of blood vessels. (I don't know how much and I'm too lazy to look it up now.) The vessels that take blood from the heart to the body are arteries and the ones that return thee blood to the heart are called veins. In humans the veins in the legs are equipped with one way valves that help keep the blood from falling back down to the feet. If these valves do not close completely or do not close at all gravity takes over and the blood pools in the lower veins. This can be very uncomfortable (achy, burning, itchy) and is often visible in the form of spider veins and vericose veins.Like breast cancer this is more commonly found in women who may "earn" them as part of the birthing process but can also affect men. The main cause of varicose veins and venous insufficiency in general is genetics. However, symptoms can be exacerbated by long periods of inactivity, hours and hours on your feet, or sitting for prolonged periods of time.
The human body has miles and miles of blood vessels. (I don't know how much and I'm too lazy to look it up now.) The vessels that take blood from the heart to the body are arteries and the ones that return thee blood to the heart are called veins. In humans the veins in the legs are equipped with one way valves that help keep the blood from falling back down to the feet. If these valves do not close completely or do not close at all gravity takes over and the blood pools in the lower veins. This can be very uncomfortable (achy, burning, itchy) and is often visible in the form of spider veins and vericose veins.Like breast cancer this is more commonly found in women who may "earn" them as part of the birthing process but can also affect men. The main cause of varicose veins and venous insufficiency in general is genetics. However, symptoms can be exacerbated by long periods of inactivity, hours and hours on your feet, or sitting for prolonged periods of time.Options:
 Temporary solutions to the pain and discomfort include wearing compression sock/stockings and use of Ibuprofen or other NSAIDS to help with the inflammation.When these simple measures are not enough or the discomfort becomes too great, getting rid of the failing veins can be achieved through surgery.Traditionally veins were able to be "stripped" but this is a fairly invasive procedure requiring significant recovery time. One less invasive alternative is ablation. This is a process where a catheter is inserted in the vein and as it is removed sections of the failing veins are cauterized shut. For some reason I used to have the strange idea that new veins would grow in the old veins' place but that is not correct. The ablated vein gets absorbed and the blood is forces to return to the heart through the other healthier veins.
Temporary solutions to the pain and discomfort include wearing compression sock/stockings and use of Ibuprofen or other NSAIDS to help with the inflammation.When these simple measures are not enough or the discomfort becomes too great, getting rid of the failing veins can be achieved through surgery.Traditionally veins were able to be "stripped" but this is a fairly invasive procedure requiring significant recovery time. One less invasive alternative is ablation. This is a process where a catheter is inserted in the vein and as it is removed sections of the failing veins are cauterized shut. For some reason I used to have the strange idea that new veins would grow in the old veins' place but that is not correct. The ablated vein gets absorbed and the blood is forces to return to the heart through the other healthier veins. My History:
I have many relatives with varicose veins and that is most likely why I have mine but I didn't always have them. My first recollection of having any strange visible veins in my legs is from shortly after I was hit by a car in 2002. It was a minor hit where I was more concerned about my Discman than my body and no medical or legal attention was given. But during the collision my right shin collided with the car's bumper. Soon after I noticed it was a little purple and was tender. I thought this was a bruise but in the ensuing years it has turned into what I affectionately call my 3D tribal tattoo, my biggest, grossest, most noticeable, and most painful varicose vein.
 | |
| 1/2/2013 |
 |
| 1/2/2013 |
In the summer of 2012 I finally caved and went in for the ultrasound. Dr Grover took pictures and did and ultrasound on both legs, both upper and lower. I had always thought that the problem was just what I was able to see but we found out that I had venous insufficiency in both legs both upper and lower. In order to test the veins they push on your leg to instigate blood flow and they time how long it take for the valves to close. If it take more than 1/2 second then the veins are bad enough that they are covered by insurance. I had veins that took longer in both my upper and lower legs. The fun thing: the gnarly one in my right lower leg didn't even close for 2 seconds while we watched it. We gave up waiting for it to close. I shared the news with Martha and we made arrangements to do the operations in January to eat up our insurance deductible so that any further problems for the rest of the year would be taken care of.
As we called to make the appointment, it turns out that I would have to undergo 3 separate procedures.
Procedure #1:
 | |
| Before Procedure #1: Numbing cream in saran wrap |
When I got to the office I laid down on the table and they prepped the room for the procedure. They had hospital gowns on and everything. I got to wear some briefs but other than that I was bare from the waist down. They placed a drape over my lower body but taped it to my skin so that only the inside of each leg was exposed. The doctor cleaned my legs and injected local anesthesia to the area around the veins. An IV was inserted in the vein in my calf and through the IV they inserted the catheter on a long wire. Dr Grover just fed it up the vein until it got to the top of the area to be treated. He used the ultrasound to make sure it was in the right place. Then I learned a little more about human anatomy. Did you know that the veins in your legs are housed within a sheath-like membrane? I didn't. It was cool to hear the doctor explain to the med student what he was doing and I asked a bunch of questions.Anyway, because the catheter gets so hot to cauterize the vein closed, they inject fluid between the vein and the sheath to have a buffer zone to avoid damage to surrounding tissues. This creates pressure and is kind of uncomfortable in a strange way. Once the flluid and catheter are in place, they cauterize a small section at a time as they work their way out of the leg. Then the whole process is repeated on the other leg. I remained alert and awake during the whole procedure and was only a little uncomfortable a couple of times.
 |
| The line and punctures from injecting fluid |
 |
| Irritated thigh skin from the tape |
 |
| Mummy legs after Procedure #1 |
Once I was all cleaned up, The doctor wrapped my legs from foot to crotch with ace bandages that I had to wear until the next morning. This quickly became uncomfortable as the bandages seemed to bunch up behind my knees and pinch my skin and pull my hairs. I went home and rested but I did go for a 20 minute easy walk later that evening.
 | |
| The wrappings |
 |
| The mummy unwrapped |
 | |
| My new thigh high compression Stockings |
Monday I went for my first run. To make sure I kept it easy I wore my heart rate monitor. I went 6 miles which was probably a little far but I felt ok. My legs just felt a little off. Monday afternoon I had my post-op checkup and got mapped for my next procedure which we thought would be done Tuesday. We thought wrong and scheduled it for Today (1/10/13).
 |
| Finding veins for Procedure #2: (Photo Credit Dillan) |
 |
| Mapping veins for Procedure #2 (Photo Credit Dillan) |